Why Mental Health Practices in Rhode Island Are Rethinking Their Billing Strategy
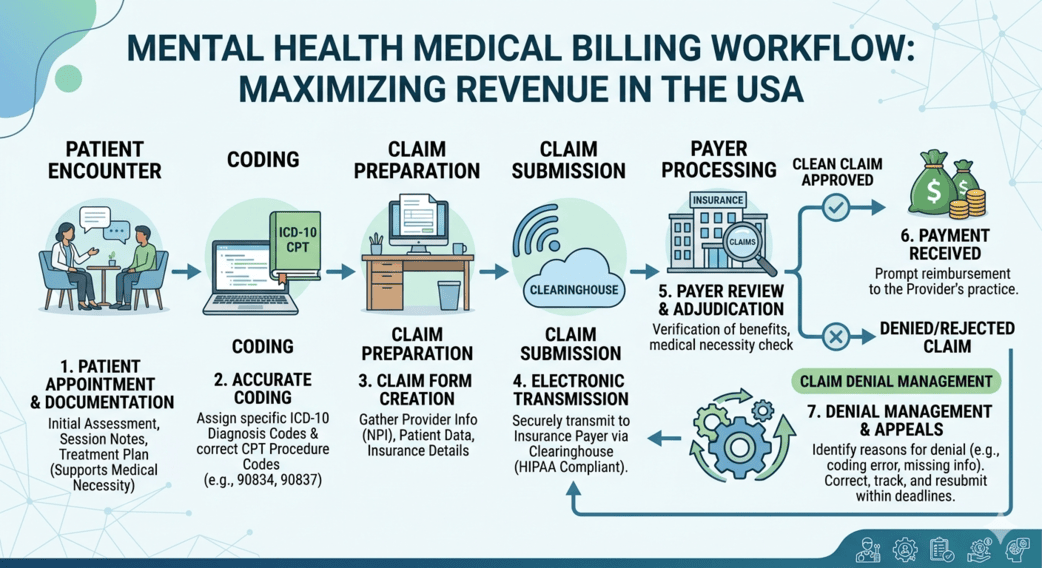
Mental health providers across Rhode Island are facing a quiet but persistent challenge—getting paid accurately and on time. While the demand for behavioral health services continues to grow, the complexity of insurance requirements, coding rules, and reimbursement policies has also increased. Many therapists, psychiatrists, and group practices find themselves spending more time on administrative tasks than on patient care.
This is where mental health billing services Rhode Island practices rely on are becoming less of a luxury and more of a necessity. From navigating payer-specific rules to reducing claim denials, specialized billing support can significantly improve financial stability while allowing clinicians to focus on what truly matters—patient outcomes.
The Hidden Complexity Behind Mental Health Billing
At first glance, billing might seem like a straightforward process: submit a claim, get reimbursed. In reality, mental health insurance billing involves multiple layers of complexity.
Unlike other medical specialties, behavioral health services often include:
- Time-based CPT codes
- Frequent policy changes across payers
- Strict documentation requirements
- Pre-authorization protocols
- Coverage limitations depending on diagnosis and provider type
A small error—such as incorrect modifiers or missing documentation—can lead to delays or outright denials. This is why many practices are now turning to mental health insurance billing services that understand these nuances in depth.
A Day in the Life: When Billing Becomes Overwhelming
Consider a mid-sized therapy clinic in Providence. The clinicians are fully booked, seeing patients back-to-back. Meanwhile, the administrative team struggles to keep up with:
- Verifying insurance eligibility
- Submitting claims across multiple payers
- Following up on unpaid claims
- Managing patient billing inquiries
Over time, delayed reimbursements start affecting cash flow. The clinic owner realizes that hiring an in-house team may not be enough—they need a mental health billing specialist who understands payer behavior and coding intricacies.
This is a common turning point where practices begin to explore outsourced solutions.
Why Outsourcing Is Gaining Momentum
Choosing to outsource mental health billing services is not just about reducing workload—it’s about improving efficiency and revenue outcomes.
What makes outsourcing effective?
First, it brings in expertise that is often difficult to build internally. A mental health billing and coding company typically employs certified professionals who stay updated on payer changes, ICD-10 updates, and compliance requirements.
Second, it introduces accountability. Unlike in-house teams juggling multiple roles, a dedicated mental health billing services agency focuses entirely on optimizing the billing process.
Finally, outsourcing offers scalability. Whether you're a solo therapist or a multi-location practice, a mental health billing provider can adjust resources based on your growth.
Key Benefits You Can Expect
Improved Claim Accuracy
Accurate coding is the backbone of successful reimbursement. A mental health medical billing services provider ensures that claims are submitted correctly the first time, reducing rejection rates.
Faster Payments
With systematic follow-ups and denial management, outsourced mental health billing teams help accelerate payment cycles.
Reduced Administrative Burden
Delegating billing tasks allows clinicians and staff to focus on patient care instead of paperwork.
Better Compliance
Regulatory requirements in mental health billing are constantly evolving. A mental health billing consultant ensures your practice stays compliant with state and federal guidelines.
What Sets a Great Billing Partner Apart?
Not all billing providers deliver the same value. If you’re searching for the best mental health billing agency, here are a few qualities to prioritize:
Industry-Specific Expertise
A general billing service may not fully understand the nuances of behavioral health. Look for a mental health billing agency with proven experience in psychiatry, therapy, and counseling services.
Transparent Reporting
Clear insights into claims, denials, and revenue trends help you make informed decisions.
Customized Solutions
Every practice operates differently. The right mental health medical billing solution should align with your workflows and goals.
Strong Communication
You should never feel in the dark about your revenue cycle. The top outsource mental health billing company will maintain consistent communication and provide actionable insights.
Common Challenges in Rhode Island—and How to Overcome Them
Mental health providers in Rhode Island face unique challenges due to varying payer requirements and regional policies.
Challenge 1: Insurance Variability
Different insurers have different reimbursement rules. A professional mental health billing company can track these variations and ensure accurate submissions.
Challenge 2: High Denial Rates
Denied claims are not just frustrating—they’re costly. A reliable mental health billing companies partner will identify patterns and fix root causes.
Challenge 3: Time Constraints
Clinicians often lack the time to manage billing effectively. This is where billing services for mental health therapists become invaluable.
Practical Tips for Improving Your Billing Process
Even if you’re considering outsourcing, there are steps you can take right now to strengthen your billing workflow:
1. Verify Insurance Before Every Visit
Eligibility checks reduce surprises and ensure smoother claim processing.
2. Maintain Detailed Documentation
Incomplete notes can lead to claim denials or audits.
3. Track Key Metrics
Monitor denial rates, reimbursement timelines, and collection percentages.
4. Invest in Training
If you have an in-house team, regular training is essential to keep up with coding changes.
5. Evaluate Outsourcing Options
If billing continues to strain your resources, partnering with a best outsource mental health billing and coding company could be the right move.
When Does It Make Sense to Outsource?
Not every practice needs to outsource immediately. However, certain signs indicate it might be time:
- Frequent claim denials
- Delayed reimbursements
- Increasing administrative workload
- Difficulty keeping up with compliance updates
At this stage, transitioning to mental health medical billing services outsourcing can provide both relief and measurable improvements in revenue.
The Bigger Picture: Revenue Cycle Optimization
Billing is just one part of the financial ecosystem. To truly maximize revenue, practices need a comprehensive approach that includes:
- Accurate patient intake
- Efficient claims submission
- Proactive denial management
- Timely patient collections
This is where billing services for mental health providers integrate into a broader strategy—often referred to as revenue cycle optimization.
How the Right Partner Transforms Your Practice
A well-chosen mental health billing services agency doesn’t just process claims—it transforms how your practice operates financially.
Imagine:
- Predictable cash flow
- Reduced administrative stress
- Higher reimbursement rates
- More time for patient care
These outcomes are not theoretical—they’re achievable with the right expertise and systems in place.
FAQs
What are mental health billing services?
Mental health billing services handle the submission, tracking, and management of insurance claims for behavioral health providers, ensuring accurate and timely reimbursements.
Why is mental health billing more complex than other specialties?
It involves time-based codes, strict documentation requirements, and varying insurance policies, making it more intricate than many other medical fields.
Should I outsource my mental health billing?
If your practice faces frequent denials, delayed payments, or administrative overload, outsourcing can significantly improve efficiency and revenue.
How do I choose the right billing company?
Look for experience in behavioral health, transparent reporting, strong communication, and customizable solutions tailored to your practice.
What services are typically included?
Most providers offer claim submission, denial management, payment posting, insurance verification, and reporting.
Closing Thoughts: Building a Sustainable Financial Future
Mental health practices in Rhode Island are at a critical intersection—growing demand on one side and increasing administrative complexity on the other. Navigating this landscape requires more than just effort; it requires the right systems and expertise.
Whether you’re a solo therapist or managing a multi-provider clinic, investing in the right billing strategy can reshape your financial health. From leveraging specialized mental health insurance billing expertise to adopting a complete revenue cycle approach, the goal is simple: reduce friction and improve outcomes.
Organizations like 247 Medical Billing Services are helping practices bridge this gap by offering integrated support that goes beyond basic claims processing. By combining medical billing services, medical coding services, and medical billing and coding services with comprehensive revenue cycle management and credentialing services, they enable providers to operate with clarity and confidence.
In the end, the right billing partner doesn’t just improve your bottom line—it gives you the freedom to focus on the work that matters most: delivering quality mental health care.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Giochi
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Altre informazioni
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


