Why Mental Health Practices in Pennsylvania Are Turning to Specialized Billing Support
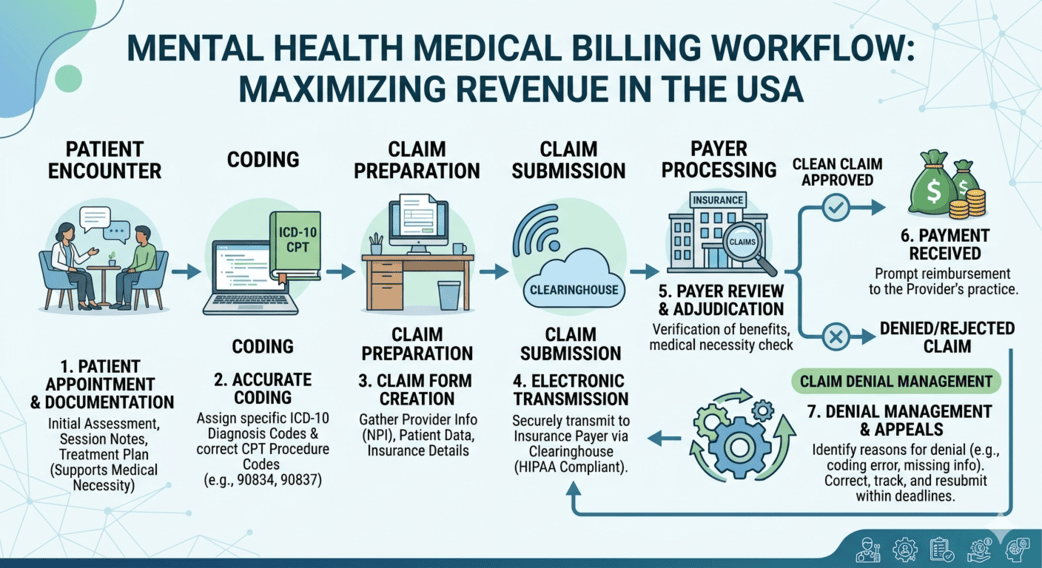
Mental health providers across Pennsylvania are facing a difficult balancing act. On one side, there’s a growing demand for therapy, psychiatry, counseling, and behavioral health services. On the other, insurance rules, coding updates, prior authorization requirements, and delayed reimbursements continue to create administrative pressure that many practices simply weren’t built to handle.
For independent therapists, group practices, psychologists, and psychiatric clinics, billing has become more than just a back-office task. It directly affects cash flow, patient experience, compliance, and long-term growth. That’s one reason the demand for mental health billing services Pennsylvania providers can rely on has increased significantly in recent years.
Whether it’s navigating Medicaid regulations, handling denied claims from commercial payers, or managing telehealth reimbursement changes, mental health practices need systems that work efficiently without draining valuable clinical time.
This article explores why specialized billing support matters, what providers should look for in a billing partner, and how outsourced billing solutions are helping Pennsylvania mental health practices improve operations and revenue performance.
The Administrative Burden Behind Mental Health Care
Behavioral health billing is different from general medical billing. Therapy sessions, psychiatric evaluations, medication management, intensive outpatient programs, and telehealth visits all come with their own coding complexities and payer-specific rules.
A therapist may spend an hour helping a patient manage anxiety or trauma, only to later discover that a claim was denied because of a modifier issue, incorrect authorization, or documentation inconsistency.
For many practices, the real challenge isn’t patient care. It’s everything that happens afterward.
Common issues mental health providers face include:
- Frequent claim denials tied to authorization requirements
- Delayed reimbursements from Medicaid managed care plans
- Complex CPT coding for psychotherapy sessions
- Insurance eligibility verification challenges
- Documentation requirements for behavioral health claims
- Telehealth billing regulation changes
- Coordination of benefits complications
Without dedicated expertise, these issues can quickly disrupt revenue cycles.
That’s why many clinics now work with billing services for mental health providers that understand the unique workflow of behavioral healthcare instead of using generalized billing support.
Why Pennsylvania Mental Health Practices Need Specialized Billing Expertise
Pennsylvania has a diverse payer landscape that includes commercial insurers, Medicaid plans, Medicare, and regional healthcare networks. Each payer may interpret mental health billing guidelines differently.
For example, one insurer may require strict session time documentation for psychotherapy claims, while another focuses heavily on diagnosis specificity or authorization timelines.
A generalized billing team often struggles with these nuances.
A specialized mental health billing and coding company understands:
- Behavioral health CPT and ICD-10 coding
- Psychiatry-specific modifiers
- Telehealth compliance updates
- State-specific payer requirements
- Documentation standards for audits
- Coordination between clinicians and billing staff
This expertise reduces avoidable errors and helps practices maintain healthier reimbursement cycles.
When In-House Billing Starts Holding a Practice Back
Many practices initially manage billing internally. In smaller offices, therapists or administrative staff may submit claims themselves. While this can work temporarily, growth usually exposes operational gaps.
Consider a small counseling center in Pennsylvania with four therapists. As patient volume increases, front-desk staff become overwhelmed with scheduling, insurance verification, patient calls, and claims follow-up. Denials begin piling up. Payments slow down. Staff burnout increases.
The problem isn’t necessarily poor effort. It’s lack of specialization and bandwidth.
This is often the point where practices begin exploring outsourced mental health billing solutions.
Outsourcing allows providers to shift administrative pressure to experienced professionals who focus exclusively on behavioral health reimbursement processes.
What a Strong Mental Health Billing Partner Actually Does
Not all billing companies offer the same level of service. Some simply submit claims. Others actively optimize revenue performance and compliance.
High-performing mental health billing companies typically provide support across the entire reimbursement cycle.
Insurance Verification and Eligibility Checks
Coverage errors are one of the leading causes of denied behavioral health claims. Effective billing teams verify benefits before appointments occur, reducing unexpected claim issues later.
This includes confirming:
- Session limits
- Copays and deductibles
- Authorization requirements
- Telehealth eligibility
- Covered behavioral health services
Accurate Coding and Claim Submission
Behavioral health coding demands precision. Small errors can lead to delays, audits, or underpayments.
Experienced teams handling billing services for mental health therapists understand how to correctly code:
- Individual psychotherapy
- Family therapy
- Group counseling
- Psychiatric diagnostic evaluations
- Medication management
- Crisis intervention services
Proper coding improves clean claim rates and speeds reimbursement.
Denial Management
Denied claims are not always final. Skilled billing teams analyze denial patterns, correct issues, and aggressively pursue appeals where appropriate.
A proactive mental health billing agency doesn’t just resubmit claims randomly. It identifies root causes and prevents recurring issues.
Accounts Receivable Follow-Up
Outstanding claims can quietly drain a practice’s revenue if left unmanaged. Effective follow-up processes help reduce aging accounts receivable and improve collections.
The Financial Impact of Outsourced Mental Health Billing
Many providers hesitate to outsource because they worry about costs. Ironically, poor billing processes often cost far more than outsourcing itself.
Missed claims, delayed reimbursements, coding errors, and uncollected balances create substantial revenue leakage over time.
A practice that improves claim acceptance rates from 82% to 95% can experience a major increase in monthly cash flow without adding additional patients.
That’s one reason mental health medical billing services outsourcing has become increasingly common among growing behavioral health organizations.
Outsourcing can help practices:
- Reduce denied claims
- Improve reimbursement speed
- Increase collections
- Lower staffing burdens
- Improve reporting accuracy
- Reduce compliance risks
The result is often a more financially stable practice with fewer operational disruptions.
Telehealth Changed Behavioral Health Billing Permanently
The rise of teletherapy transformed mental healthcare delivery across Pennsylvania. While telehealth expanded patient access, it also introduced new billing complexities.
Providers suddenly had to navigate:
- Telehealth modifiers
- POS coding changes
- Audio-only billing rules
- Cross-state licensure concerns
- Changing payer reimbursement policies
Many practices struggled to keep up with evolving requirements.
A specialized mental health billing consultant can help providers adapt to these changes while maintaining compliance and reimbursement accuracy.
Even now, telehealth billing regulations continue evolving. Practices that fail to monitor payer updates risk denials and payment delays.
Small Practices vs. Large Behavioral Health Organizations
Billing challenges look different depending on practice size.
Independent Therapists
Solo practitioners often lack administrative support. They may spend evenings handling claims instead of focusing on patient care or professional growth.
For these providers, outsourced mental health billing creates time freedom while improving collections.
Group Practices
Larger therapy groups face more operational complexity. Multiple providers, credentialing timelines, insurance contracts, and reporting needs require stronger billing infrastructure.
A scalable mental health billing and coding company can support growth without forcing providers to constantly expand internal staffing.
Community Mental Health Clinics
Organizations serving Medicaid-heavy populations often face additional compliance and authorization challenges. Specialized billing expertise becomes critical for maintaining reimbursement consistency.
Choosing the Right Billing Company Matters
The billing partner a practice chooses can significantly influence financial performance.
Not every company claiming behavioral health expertise truly understands the field.
When evaluating a top outsource mental health billing company, providers should ask questions like:
- Do they specialize in behavioral health?
- Are they familiar with Pennsylvania payer policies?
- How do they handle denied claims?
- What reporting tools do they provide?
- How transparent is their communication?
- Do they support credentialing and enrollment?
- What experience do they have with telehealth billing?
A strong partnership should feel collaborative rather than transactional.
Compliance Is No Longer Optional
Behavioral health documentation and billing are heavily scrutinized. Audits, payer reviews, and compliance investigations can create serious financial and legal risks.
Incorrect coding, inadequate documentation, or improper billing practices may lead to recoupments or penalties.
Experienced mental health billing companies help practices stay aligned with evolving standards by:
- Monitoring coding updates
- Reviewing claim accuracy
- Supporting audit readiness
- Maintaining HIPAA-compliant workflows
- Ensuring proper modifier usage
Compliance-focused billing support protects both revenue and reputation.
The Hidden Burnout Factor
One issue rarely discussed openly is administrative burnout among mental health providers.
Many therapists enter the profession to help people, not to spend hours fighting insurance denials or chasing unpaid claims.
Over time, billing stress contributes to exhaustion and reduced job satisfaction.
Outsourced mental health billing allows clinicians to redirect energy toward patient care, supervision, and practice development instead of administrative firefighting.
For many providers, the emotional relief is just as valuable as the financial improvement.
Technology Alone Is Not Enough
Some practices assume software will solve billing problems automatically. While practice management platforms and EHR systems are helpful, technology still requires human oversight.
Claims can still be denied because of:
- Incorrect coding logic
- Missing authorizations
- Documentation inconsistencies
- Payer policy changes
- Data entry errors
The most effective systems combine modern technology with experienced billing professionals who understand behavioral healthcare reimbursement inside and out.
That’s why practices often benefit more from a knowledgeable billing team than from software alone.
Questions Providers Often Ask Before Outsourcing
Will outsourcing reduce control over my billing?
Not necessarily. Reputable billing companies provide detailed reporting, transparent communication, and real-time access to financial performance data.
Is outsourcing only for large practices?
No. Solo therapists and small counseling practices often benefit significantly because outsourcing reduces administrative strain without requiring additional in-house staff.
How quickly can results improve?
While every practice is different, many providers notice improvements in claim acceptance rates, collections, and cash flow within a few billing cycles.
Can billing companies help with credentialing?
Many providers prefer companies that also offer credentialing support because payer enrollment delays can significantly affect revenue timelines.
FAQs
What are mental health billing services?
Mental health billing services handle insurance claims, coding, payment posting, denial management, and reimbursement processes specifically for behavioral health providers such as therapists, psychologists, psychiatrists, and counseling centers.
Why is behavioral health billing more complex than general medical billing?
Behavioral health billing often involves time-based CPT codes, authorization requirements, telehealth modifiers, documentation standards, and payer-specific mental health regulations that require specialized expertise.
How can outsourced mental health billing improve revenue?
Outsourcing helps reduce coding errors, improve claim acceptance rates, speed up reimbursements, and strengthen accounts receivable follow-up, leading to healthier cash flow.
Do mental health billing companies work with Pennsylvania Medicaid plans?
Many specialized companies do. Providers should confirm that the billing team has experience with Pennsylvania-specific Medicaid managed care organizations and regional payer requirements.
What should I look for in a mental health billing consultant?
Look for experience in behavioral health coding, denial management, telehealth billing, compliance support, reporting transparency, and payer credentialing expertise.
Is outsourcing billing secure for patient information?
Reputable billing providers use HIPAA-compliant systems and secure workflows to protect patient data and maintain confidentiality standards.
Building a More Sustainable Mental Health Practice
Behavioral health providers are under increasing pressure to deliver quality care while navigating a reimbursement environment that grows more complicated every year. Administrative inefficiencies, denied claims, and staffing limitations can quietly undermine even the most dedicated practices.
That’s why specialized mental health billing services Pennsylvania providers can depend on are becoming essential rather than optional. The right billing support does more than process claims. It strengthens financial stability, improves operational efficiency, and gives clinicians more time to focus on patients.
For practices seeking long-term growth, partnering with experienced professionals in medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services can create a stronger operational foundation.
Organizations like 247 Medical Billing Services continue supporting healthcare providers with specialized billing expertise tailored to evolving industry demands. For mental health practices looking to reduce administrative stress while improving reimbursement performance, working with an experienced billing partner can be an important step toward sustainable growth and better patient care.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Spellen
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


