Medical Billing for Mental Health in the USA: Complete Guide to Compliance, Coding, and Revenue Optimization
Mental health services are becoming more important than ever across the United States. As more individuals seek therapy, psychiatric care, and behavioral health support, providers face increasing administrative responsibilities. One of the most complex parts of running a successful practice is medical billing for mental health.
Unlike general medical billing, mental health billing and credentialing services involves unique documentation standards, strict compliance requirements, therapy session coding, and payer-specific rules. Small mistakes in coding or claim submission can lead to denials, delayed reimbursements, or compliance issues.
For clinics, therapists, and psychiatrists, understanding how billing for mental health services works is essential for maintaining steady revenue and reducing administrative stress.
Why Medical Billing for Mental Health is More Complex
Mental health providers face several challenges when handling billing internally. Insurance companies have strict requirements for documentation, session duration, and medical necessity.
Some of the common complexities include:
• Therapy session time-based coding requirements
Mental health CPT codes often depend on the length of the therapy session, which requires accurate documentation.
• Strict payer policies and authorization requirements
Insurance providers may require prior authorization for certain behavioral treatments.
• Complex documentation for medical necessity
Claims must clearly justify treatment plans, progress notes, and diagnoses.
• High claim denial rates
Errors in coding and documentation frequently lead to rejected claims.
Because of these factors, many providers rely on mental health billing services to ensure accurate claim submission and timely reimbursement.
Understanding Medical Billing for Mental Health Providers
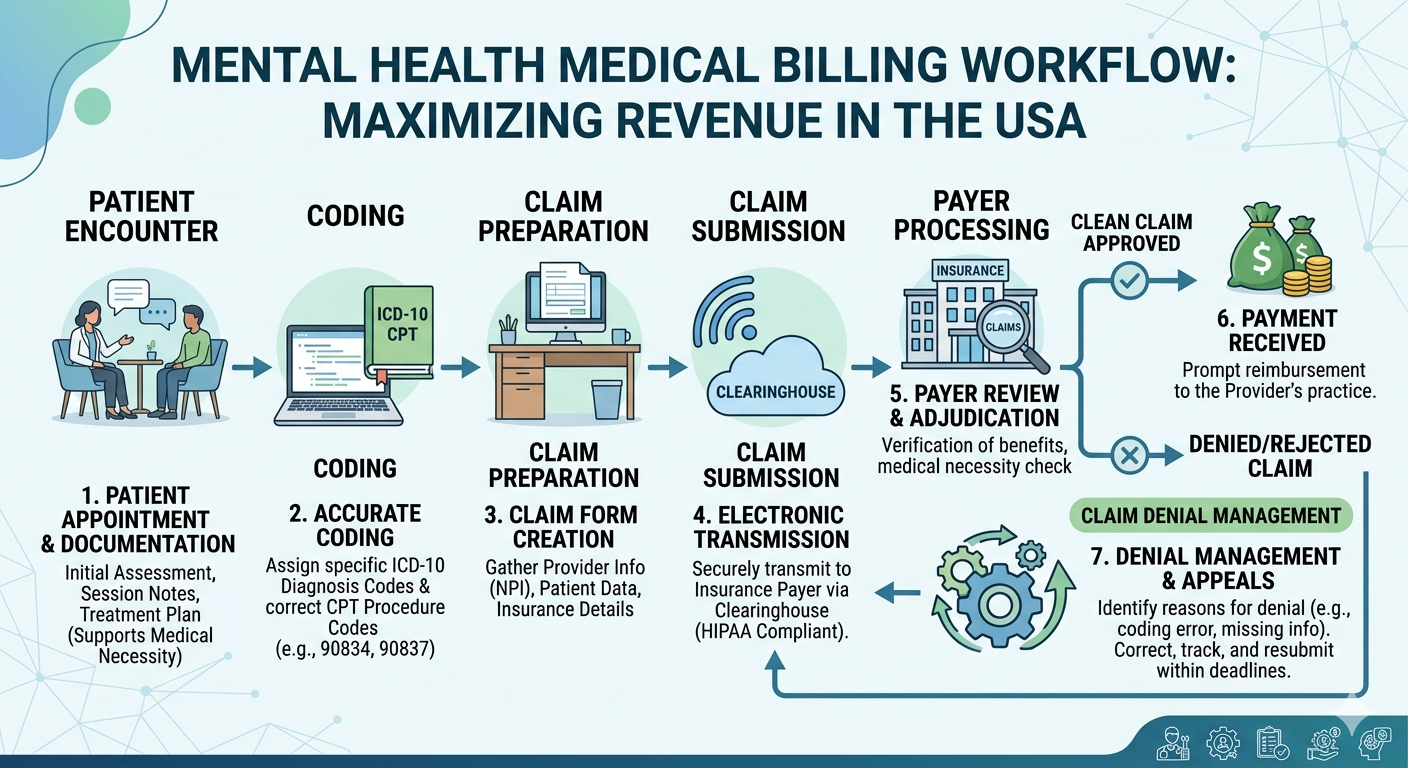
Medical billing for mental health providers involves several steps that must be carefully managed to avoid payment delays.
The typical billing process includes:
Patient insurance verification
Before treatment begins, eligibility and coverage details must be confirmed to avoid claim denials.
Accurate diagnosis coding
Mental health conditions are coded using ICD-10 diagnosis codes.
Therapy procedure coding
Sessions are reported using CPT codes based on therapy duration and type.
Claim submission to insurance payers
Clean claims must be submitted electronically with complete documentation.
Payment posting and reconciliation
Payments from insurance companies are recorded and matched with submitted claims.
Denial management and appeals
Denied claims are reviewed, corrected, and resubmitted when necessary.
Efficient coding and billing for mental health services ensures providers receive appropriate reimbursement while maintaining compliance.
Key CPT Codes Used in Mental Health Billing
Proper coding is the foundation of successful mental health medical billing. Mental health professionals rely on specific CPT codes that represent psychotherapy sessions and related services.
Some commonly used therapy codes include:
90832 – Psychotherapy session lasting approximately 30 minutes
90834 – Psychotherapy session lasting approximately 45 minutes
90837 – Psychotherapy session lasting approximately 60 minutes
90791 – Psychiatric diagnostic evaluation without medical services
90792 – Psychiatric diagnostic evaluation with medical services
These codes must match the documented session time and treatment details. Incorrect coding is one of the primary reasons claims are denied.
Professional mental health billing specialist companies ensure accurate coding and proper documentation to reduce billing errors.
Medicare Billing Rules for Mental Health Services
Many providers treat Medicare beneficiaries, making it important to understand billing Medicare for mental health services.
Medicare covers several behavioral health services including psychotherapy, psychiatric evaluations, and medication management.
Key Medicare considerations include:
Coverage for outpatient mental health therapy
Therapy services must be medically necessary and documented properly.
Co-insurance requirements
Patients are typically responsible for a percentage of the approved amount.
Telehealth mental health services
Medicare now allows many therapy sessions to be delivered through telehealth.
Documentation standards
Providers must maintain clear records that support treatment necessity.
Because Medicare billing rules frequently change, many practices rely on billing companies for mental health to stay compliant.
Benefits of Outsourcing Mental Health Billing
Handling billing internally can consume valuable time that providers would rather spend with patients. This is why many practices choose outsourcing mental health billing.
Outsourced billing services allow healthcare providers to focus on clinical care while experts manage claims and reimbursements.
Key benefits include:
Improved claim accuracy
Professional billing teams reduce coding errors and rejected claims.
Faster reimbursements
Clean claims lead to quicker insurance payments.
Lower administrative workload
Providers and staff spend less time on billing tasks.
Better denial management
Billing experts track and resolve denied claims efficiently.
Improved compliance with payer rules
Experienced teams stay updated with changing insurance policies.
Many clinics prefer outsourced billing for mental health because it improves financial stability and reduces operational stress.
Choosing the Right Mental Health Billing Company
Selecting the right partner is crucial for maintaining consistent revenue and compliance. The best mental health billing company should understand behavioral healthcare billing requirements and payer guidelines.
When evaluating billing companies for mental health, providers should consider:
Industry experience in behavioral health billing
Knowledge of CPT and ICD coding for psychotherapy services
Compliance with HIPAA and payer regulations
Transparent reporting and revenue tracking
Denial management expertise
A reliable mental health billing services company helps practices increase collections while maintaining billing accuracy.
Services Offered by Mental Health Billing Companies
A professional mental health billing company typically provides a full range of services designed to streamline revenue cycle operations.
These services may include:
Insurance eligibility verification
Claim creation and electronic submission
Coding and billing for mental health services
Payment posting and reconciliation
Denial analysis and appeals
Accounts receivable follow-up
Financial reporting and analytics
Some organizations also offer mental health billing and credentialing services, ensuring providers are properly enrolled with insurance networks before submitting claims.
For clinics looking to reduce administrative costs, outsourcing mental health billing and coding can be a strategic business decision.
Billing Challenges Faced by Mental Health Therapists
Therapists and counselors often struggle with billing due to limited administrative support.
Common issues include:
Incomplete documentation leading to claim rejections
Difficulty understanding insurance reimbursement policies
Time spent managing claims instead of patient care
Tracking payer-specific therapy coding requirements
Many therapists choose billing services for mental health therapists to handle these challenges professionally.
Mental Health Billing for Clinics and Group Practices
Larger practices and behavioral health clinics often deal with a higher volume of claims and multiple providers.
Billing services for mental health clinics help streamline operations by managing:
Multi-provider claim submissions
Insurance payer communication
Credentialing and provider enrollment
Financial reporting and revenue analysis
Partnering with a top mental health billing company helps clinics improve operational efficiency while maintaining consistent cash flow.
Cost Considerations When Outsourcing Billing
Cost is one of the main concerns for healthcare providers when choosing a billing partner.
While some providers search for a cheap outsource mental health billing company, it is important to prioritize experience, accuracy, and compliance.
Low-cost services may lead to coding errors, compliance risks, and increased claim denials.
Instead, providers should look for the best outsource mental health billing and coding services that offer transparent pricing and measurable performance improvements.
The right partner will improve revenue collection and reduce administrative burden, making the investment worthwhile.
The Role of Technology in Modern Mental Health Billing
Technology has transformed the way billing for mental health providers is handled.
Advanced billing systems now include:
Automated claim submission tools
Real-time insurance verification
Integrated electronic health records
Denial tracking systems
Revenue analytics dashboards
These tools help improve billing accuracy and speed up reimbursement cycles.
Modern mental health billing solutions allow providers to focus on delivering quality care while maintaining efficient financial operations.
How Professional Billing Improves Practice Growth
Efficient mental health billing directly impacts the financial health of a practice.
When billing processes run smoothly, providers benefit from:
Higher claim approval rates
Reduced administrative costs
Improved revenue cycle management
Better patient billing transparency
More time dedicated to patient care
This is why many organizations partner with a trusted mental health billing company to optimize their financial performance.
Professional behavioral and mental health billing services help ensure compliance, reduce claim errors, and maximize reimbursements.
Conclusion
The growing demand for behavioral healthcare has made efficient medical billing for mental health more important than ever. Providers must manage complex coding systems, insurance policies, and strict documentation standards while focusing on patient care.
By partnering with experienced mental health billing specialist companies, therapists, psychiatrists, and clinics can improve claim accuracy, reduce denials, and maintain consistent revenue flow.
Healthcare organizations seeking reliable support often choose expert partners like 247 Medical Billing Services, which provides comprehensive medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. With a strong focus on compliance and efficiency, professional billing partners help mental health providers streamline operations and focus on delivering high-quality patient care.
Frequently Asked Questions
What is medical billing for mental health?
Medical billing for mental health refers to the process of submitting and managing insurance claims for psychotherapy, psychiatric care, counseling sessions, and other behavioral health treatments. It involves accurate coding, claim submission, and reimbursement tracking.
Why do mental health providers outsource billing services?
Many providers choose outsourcing mental health billing to reduce administrative workload, improve claim accuracy, and ensure compliance with insurance payer requirements.
What services do mental health billing companies provide?
Mental health billing services typically include insurance verification, claim submission, coding support, denial management, payment posting, and financial reporting.
How does coding impact mental health billing?
Correct CPT and ICD coding ensures that therapy sessions are accurately documented and reimbursed by insurance providers. Coding errors are a common cause of claim denials.
Is Medicare coverage available for mental health services?
Yes, Medicare covers many behavioral health services including therapy sessions, psychiatric evaluations, and telehealth mental health care when medically necessary and properly documented.
How do I choose the best mental health billing company?
Providers should look for companies with experience in behavioral health billing, strong compliance practices, transparent reporting, and proven expertise in coding and billing for mental health services.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- الألعاب
- Gardening
- Health
- الرئيسية
- Literature
- Music
- Networking
- أخرى
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


